A preventable outbreak in a system that did not act in time
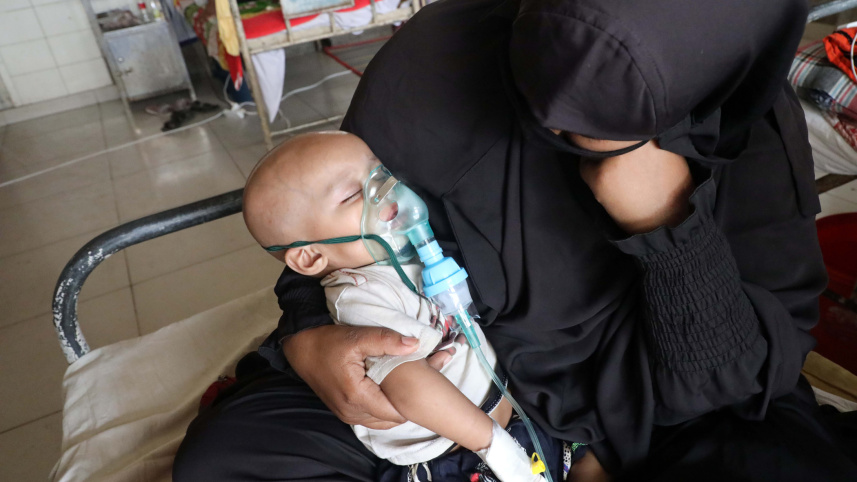
In March alone, amid a sudden measles outbreak, some 229 patients died at Rajshahi Medical College Hospital (RMCH) awaiting ICU beds. Ninety-one of the deceased were children. Many died on waiting lists, never receiving the treatment they needed, and the numbers are still rising.
At RMCH, the consequences of the healthcare system’s failure are not abstract. With limited ICU capacity, hundreds of patients were placed on waiting lists over the course of a single month. Some could be admitted but many were not. Access to life-saving care became dependent on whether a bed became available in time. That distance between needing care and receiving it is where the system begins to fail in a way that is both visible and irreversible.
As of early April, Bangladesh recorded 9,883 suspected measles cases and 128 suspected deaths, with 81 percent of infections among children under five and cases reported across 56 districts. Paediatric wards in several public hospitals are operating beyond capacity, while critical care units are under sustained pressure. These are not isolated developments and they are putting pressure on a system that is already struggling. Routine immunisation coverage has slipped in recent years, leaving many children unprotected. According to Unicef and WHO, post-pandemic disruptions have created pockets of “zero-dose” and under-vaccinated children—those who have missed routine vaccines entirely or partially. Measles, which requires around 95 percent immunisation coverage to interrupt transmission, does not need large gaps to spread. Even small breaks in coverage can be risky, particularly in densely populated areas where transmission accelerates quickly once it begins.
Early cases were identified in Rohingya refugee camps in Cox’s Bazar in January. Within weeks, infections were rising in highly populated slum areas in Dhaka. These outbreak locations reflect where immunisation coverage is most fragile: where it is easier to look away. The fragile condition of the healthcare system is not a new reality for Bangladesh. Adequate investment and actions in healthcare infrastructure improvement have been emphasised enough in public discourse. Despite the repeated raising of flags, budgetary allocations have been minimal, mobilisation even less so.
Public spending on health has not increased sufficiently over the years, rising from just over Tk 32,000 crore during the early pandemic period to nearly Tk 42,000 crore in the latest fiscal cycle. That might look like progress on paper, however in reality, the shift is more restricted. Health spending has remained close to five percent of the national budget, and as a share of GDP, it still accounts for less than one percent. Even within that bracket, utilisation has struggled to keep pace with allocation, with development spending frequently revised and at times shelved as projects stall in the procurement and implementation phases. The emergency vaccination campaign now underway, targeting more than a million children in high-risk districts, reflects a system that reacts to events. WHO and Unicef have warned that without rapid and sustained coverage, transmission will continue and further complications will follow.
The emergencies differ—between Covid and measles outbreaks—but the problems do not. Facilities are present, but not all are running the way they should. Staffing falls short when the number of patients rises, the system begins to falter under stress, and expansion is discussed only after a crisis emerges.
Outside Dhaka city, these limitations are more exposed. Hospitals beyond the capital handle outbreaks without the required resources. They have fewer trained specialists, outdated or limited equipment, and little room to adjust when cases rise quickly. When cases mount, patients wait for longer, conditions worsen, and whether someone gets care in time often comes down to what is available at that moment. Then, questions arise about whether healthcare in marginal areas is prioritised, about delayed investment in infrastructure upgradation and capability building, and about the absence of a consistent medical governance framework. Ultimately, it reflects negligence and a persistent apathy towards the periphery.
What makes this particularly difficult to accept is that measles remains one of the most preventable infectious diseases, yet also one of the most longstanding ones for Bangladesh. Vaccines are widely available, protocols are well-established, and the country has previously demonstrated strong immunisation performance, achieving coverage levels that significantly reduced transmission. The tools to prevent this chain from forming already exist within the system; however, what has weakened is continuity: between policy and implementation, between reported coverage and actual reach, and between early warning signals and timely response. These are governance gaps.
Declining follow-through in routine immunisation, missed cohorts of children, and uneven coverage have been visible for some years now. They were not addressed in time under the previous governments. The present response, while knee-jerk and piecemeal at best, has followed escalation rather than preventing it. What we are currently witnessing is not a sudden crisis, but a failure that was allowed to unfold without adequate containment.
The current failure is visible in the queues, in the waiting lists, and in the children who did not survive long enough to receive care. Nothing about this was unexpected. The risks were known. The sequence was clear. But it was not acted on. These deaths sit on our conscience, because the lessons were there—from past outbreaks, immunisation successes, healthcare system upgrade proposals—but the system was not reinforced to follow through or operate under pressure. We must demand urgent action to strengthen the system now to prevent further tragedy.
Tasneem Tayeb is a columnist for The Daily Star. Her X handle is @tasneem_tayeb.
Views expressed in this article are the author's own.
Follow The Daily Star Opinion on Facebook for the latest opinions, commentaries, and analyses by experts and professionals. To contribute your article or letter to The Daily Star Opinion, see our guidelines for submission.




 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel.
Comments